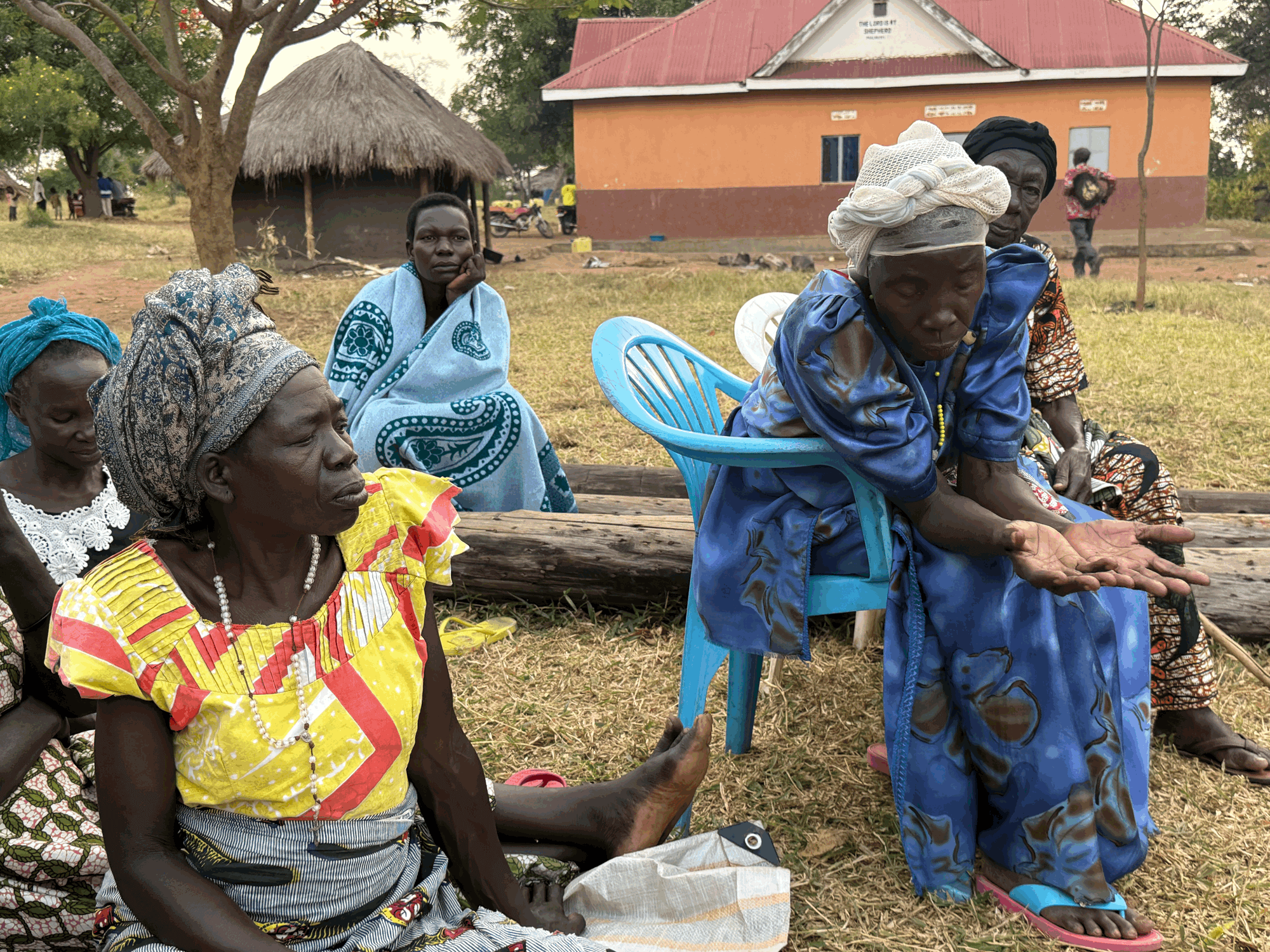Protesters demanding government resignations due to the management of the ebola crisis in Hospital Carlos III of Madrid, where a nursing assistant is being treated having become infected with the virus. Marcos del Mazo/Demotix. All rights reserved.
The ebola crisis may be entering a new and potentially hugely dangerous phase as it spreads beyond its West African epicenter, with a Liberian man having died in a Texan hospital, and a Spanish nurse critically ill with the disease in Madrid. A suspected case in Australia, concerning a nurse who had been working in Sierra Leone, has proved a false alarm, but other cases are sure to emerge. The rate of new infections has now slowed somewhat in Guinea, where the outbreak started, but the epidemic remains out of control in Liberia and Sierra Leone, with the caseload doubling every 2-3 weeks. Although the global response has now been greatly expanded, many pledges of support have yet to materialize on the ground, and the scale of the crisis continues to dwarf existing efforts to contain it.
It has been surprising to see a series of mistakes in the handling of these first cases to have been contracted outside of West Africa, given the prior knowledge of the disease and vastly superior medical facilities, compared to the poverty-stricken countries where the virus first spread. These include a failure to diagnose Liberian Eric Duncan on his initial visit to an emergency ward in Texas, and a failure to follow safety procedures when he was finally admitted. These slip-ups may well have contributed to Duncan’s death, since early detection is the key factor in surviving the disease, and they have certainly put many others at risk. There has also been criticism of the protocols followed in Spain, where sub-standard protective equipment may have caused the nurse’s infection. Human error appears to be as unavoidable in the developed world as it is in West Africa.
Far less surprising is the exponential way in which the disease is now spreading at its epicenter, which is rather the inevitable and predictable outcome of the highly inadequate international response to the outbreak. The lack of ambulances, hospital beds, and even plastic gloves have all played a role in allowing the disease to get out of control, particularly in the slums of Freetown and Monrovia.
The impact of these insufficient resources has been greatly compounded by the deep mistrust of government and other officials after decades of conflict and bad governance in the sub-region. Despite being relatively approved of by western donors, the post-war governments in Liberia and Sierra Leone have quickly reverted to the same old patterns of promising much and delivering little. The disappearance of a large chunk of a contribution from the EU to the health budget in Liberia, as reported recently, is just the tip of the iceberg.
Another legacy of the region’s volatile history is the high levels of illiteracy, which contribute to an almost wilful ignorance of the disease and the way it spreads, despite concerted information campaigns. The section of the population worst affected by ebola, 15-35 year olds, is the same demographic that missed out almost entirely on getting an education during the wars of the 1990s and early 2000s. Combined with their distrust of the authorities, this lack of education makes people more susceptible to the various conspiracy theories being promulgated, the most popular of which claims that the virus was created in a US lab and unleashed on Africa as a population control measure. Such beliefs inhibit a more rational response to the disease.
Lack of education also fuels the commonly-held belief that witchcraft is to blame for the crisis. In rural villages where the only visible signs of the twenty first century are a few plastic buckets and slippers, the odd radio, and the ubiquitous mobile phones, albeit twentieth century models, this conviction leads many to reject the explanations and advice of medical personnel in alien suits. Instead, they seek refuge in existing traditions, treating fever with local remedies and washing and preparing dead bodies in the same way they always have, even though this exposes them to the disease at its most contagious. The extent of this antipathy towards outsiders can been seen in the series of attacks on health workers by villagers in rural Guinea, where one little reported incident left 8 people dead.
The actions of the two Liberians who have carried the disease abroad may also be seen as irrational, and certainly highly destructive. Patrick Sawyer almost definitely knew he had the disease when he travelled to Nigeria, while Eric Duncan lied on an exit questionnaire which asked if he had been in contact with anyone with possible symptoms of the disease. He had helped transport a very ill pregnant neighbor on a fruitless search for a hospital bed, a woman who had died the same night from blood hemorrhaging.
But Sawyer was reportedly seeking better treatment in Nigeria and Duncan, who had no symptoms when he left Liberia, was fulfilling a long-held dream to reunite with his former girlfriend and their son in the US. His case highlights the futility of border controls in the face of the decision-making processes of individuals, and when the symptoms of the disease can take up to 21 days to appear. How many others would also lie on a form in the same circumstances, especially if they felt perfectly healthy?
Hopefully the spread of the disease outside its epicenter will be contained, using the relatively straightforward approach of ‘trace, track and treat’ that has been effective in previous outbreaks. This strategy has allowed Nigeria to contain the outbreak triggered by Sawyer, and has also been used successfully at the Firestone Rubber Plantation in Liberia. Despite their early mistakes, the US, Spain and elsewhere obviously have the capacities and resources to implement such a strategy.
What is far less certain however is whether containment is any longer possible in the rural backwaters and urban slums of the painfully poor countries where the outbreak originated. Even with sufficient resources, it is hard to see how an effective trace, track and treat campaign could now be implemented, given both the extent of the spread and the deep resistance to externally-imposed solutions. As the disease extends its global reach, the world may wake up and flood these three countries with the vast resources that they would need to try this approach. But even if this were to happen, it may now not be enough.