Thousands of people in South Africa are avoiding health facilities, shunning life-saving treatment, out of fear of being infected by coronavirus and being harassed by police.
Even mobile clinics that provide HIV, TB and contraceptive services report a huge drop in clients – possibly because all health services are now being associated with the COVID-19 response.
“Head counts at Johannesburg clinics are down by 30% to 70%,” says Francois Venter, an infectious disease doctor at Wits University’s Faculty of Health Sciences and also a member of a special committee that is advising the South African ministry of health on COVID-19.
“These clinics are delivering absolutely essential services. We are going to spend the next six months cleaning up this catastrophe – the lack of contraception leading to unintended pregnancies and an increased demand for terminations, diseases from lack of immunisations, untreated diabetes. We are likely to see a wave of mortality linked to HIV and TB.”
TB is South Africa’s biggest killer. An estimated 63,000 people die of the bacterial disease every year, followed by diabetes. The country has the world’s biggest HIV epidemic, with almost eight million South Africans living with HIV – one in five of those aged between fifteen and 49.
During the lockdown from 27 March to 1 May, thousands of people living with HIV defaulted on their antiretroviral (ARV) drugs and TB medication.
In Gauteng alone (one of South Africa’s nine provinces), almost 11,000 HIV and over 1,000 TB patients failed to collect their medicine, according to the provincial health department. New TB tests plummeted by almost half, according to the National Institute for Communicable Diseases.
The institute blames this “dramatic decline” in tests on the lockdown’s restrictions on movement and a lack of public transport. But Anele Yawa, general secretary of the Treatment Action Campaign (TAC) – a prominent activist organisation supporting people living with HIV – says many people avoided clinics because of security crackdowns.
“The militarisation of the COVID-19 response has caused fear and resistance,” said Yawa. “Many people have been shot at and harassed. Some people in rural areas have to walk a long way to fetch medicine and were afraid to do it because they did not have a permit to travel. The police and army could have approached this in a different way by showing that they were there to help communities.”
Wanted: an integrated approach
Countrywide, entire TB hospitals and wards have been converted to COVID-19 facilities while medical staff have been redeployed to the pandemic response. Many community health workers who used to trace TB defaulters have been redirected to do COVID-19 screening.
In Khayelitsha, a partly-informal township in Cape Town township, Anja Reuter, Medecins sans Frontieres’ medical manager of drug-resistant (DR) TB, says she is worried about how few new TB and DR-TB patients have been detected since the start of the pandemic.
“There is a significant overlap of COVID-19 and TB symptoms as both may present with fever, feeling unwell with a cough or tight chest,” says Reuter, but because of the focus on COVID-19, TB cases might be overlooked. “Healthcare workers need to be trained to detect both.”
She is also concerned about whether current TB patients are able to take their medication, particularly if they are going hungry: “DR-TB patients have to take up to twenty tablets, many of which cause nausea. This is very challenging on an empty stomach.”
Also, most DR-TB patients qualify for a temporary disability grant, but the government has suspended new applications for these grants because of COVID-19.
"Health facilities are seen as places of contagion"
The key question for Linda-Gail Bekker, CEO of the Desmond Tutu HIV Foundation, is “how we can integrate COVID-19 into our services, as it is an infectious disease and another health priority alongside HIV and TB.”
This foundation operates five mobile clinics that provide HIV, TB and contraceptive services to almost 100,000 people in under-served Cape Town communities. But, Bekker says, demand for their services was “almost zero” during the lockdown.
“We usually do 40 to 50 HIV tests in a day. [Last week] we were doing ten. People are worried. Health facilities are being seen as places of contagion. There is also confusion about what people are allowed to do under lockdown. Our staff also express anxiety about going into people’s homes and communities to do tests.”
Meanwhile, TAC’s Yawa is concerned about the large numbers of people who might simply stop taking their ARVs.
“When community health workers are doing screening for COVID-19 cases, they should screen for HIV and TB also,” he said. “Contact tracers looking for COVID-19 contacts should also look for people who have defaulted on HIV and TB treatment.”
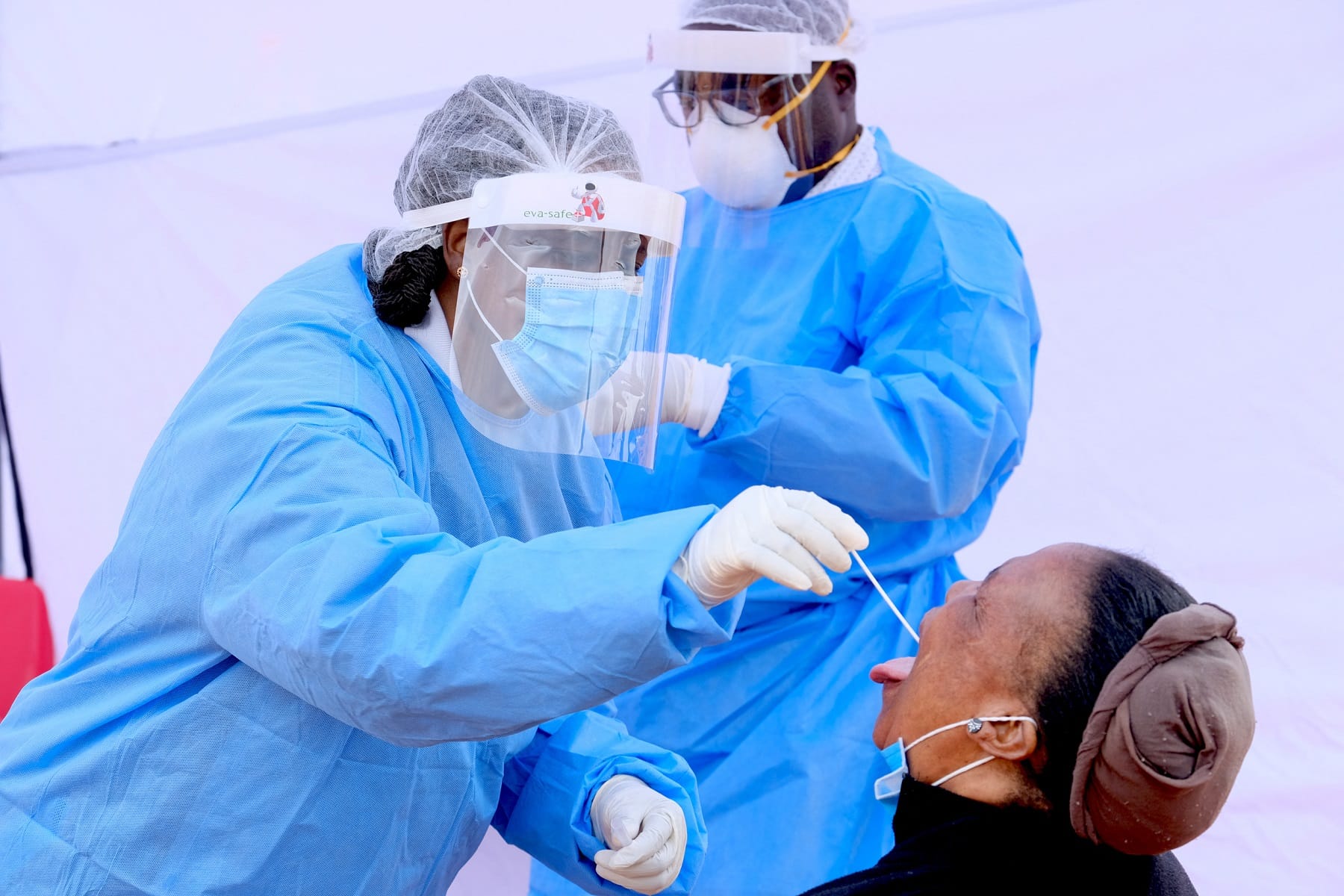
Keeping vulnerable patients safe
The Southern African HIV Clinicians Society recommends that stable HIV patients are given six months’ supply of ARVs, which would alleviate the problem of people avoiding clinics and not fetching medicine.
But this has been complicated by the fact that South Africa's national health department is in the process of changing all patients on first-line ARVs from three particular drugs to a different, less toxic combination.
Reuter says that people with TB or DR-TB are at high risk of severe COVID-19 illness, so routine clinic visits should be decreased. “But patient support needs to continue,” she adds, and this “can be done through telephonic counselling and adherence support, and patients identifying a treatment buddy or supporter at home.”
Venter and Bekker both feel much more can be done to keep people safe on public transport and in places where people congregate.
“I see red when I see people on top of each other in food queues or queuing for social grants,” says Venter. “This is where there is a role for police to enforce social distancing.”
He believes non-pharmaceutical interventions, such as handwashing and masks, should be pushed firmly: “Everyone getting on to a taxi [minibus] must get hand sanitiser, taxi drivers must wear the best masks, there must be handwashing facilities at taxi ranks.”
Bekker says she is for “smart distancing”: prohibiting large gatherings indoors such as church services and funerals.
“A long time ago, we learnt lessons about stopping the spread of TB in taxis, including by getting people to wear masks, reduce crowding and open the windows. People didn’t listen to us then but perhaps they’ll listen now.”










