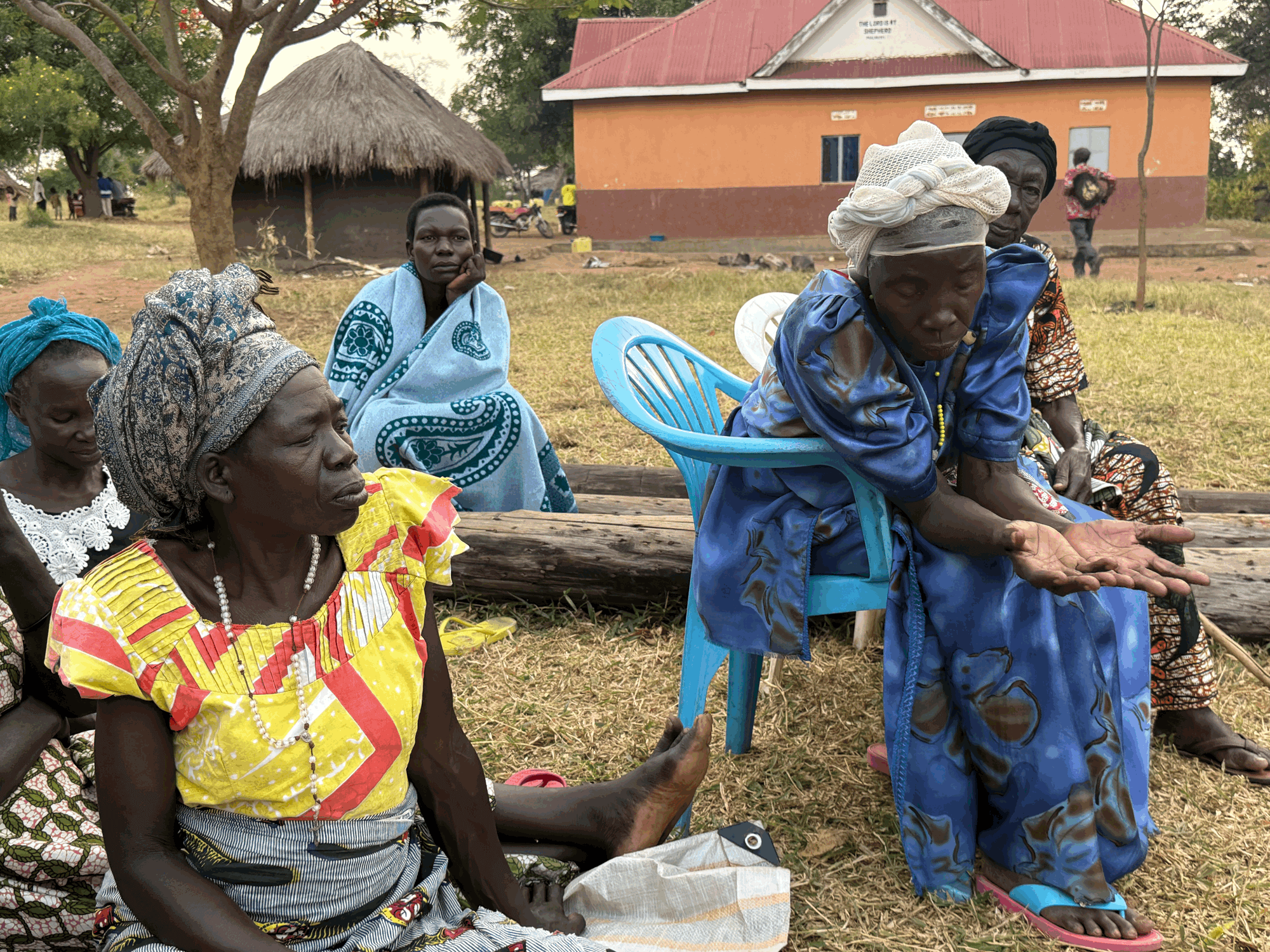This article is the sixth in 50.50's series on the World AIDS 2014 Conference taking place this week in Melbourne
One of the themes at this week's International AIDS Conference in Melbourne, is the testing and treatment of children. In Zimbabwe as elsewhere there are high numbers of children growing up with HIV who have not been diagnosed and in whom the disease is therefore advancing without check. A recently published study in Zimbabwe by the London School of Tropical Hygiene and Medicine sought to investigate why this is and how to overcome it. It concludes, “The HIV prevalence among children tested was high, highlighting the need for provider-initiated HIV testing and counselling (PITC). For PITC to be successfully implemented, clear legislation about consent and guardianship needs to be developed and structural issues addressed. Healthcare workers (HCWs) require training on counselling children and guardians, particularly male guardians, who are less likely to engage with health care services. Increased awareness of the risk of HIV infection in asymptomatic older children is needed.”
This study recommends training healthcare workers to counsel others. However, the study omitted to consider the key issue of attitudes held by health workers, lawmakers, and other professionals towards HIV and those with HIV. Unless healthworkers are offered this critical first step of training in self-awareness, to assess their own attitudes towards HIV, and therefore people with HIV, any amount of training to counsel others will be money wasted. High levels of stigma present a huge barrier across the whole spectrum of professional service providers in the field of HIV and AIDS. When will policy makers, politicians and academics start to think upstream, in order to change their own and their employees’ attitudes towards HIV before seeking to change the attitudes of others?
Stigma and discrimination are also experienced widely by many people living with HIV, particularly women and their children - in homes, communities, health-care settings, the legislative justice system and social services. This stigma is often started, and reinforced, by those who are meant to be their professional carers.
One HIV positive woman reported having been told by a healthworker, “The best thing you can do now for yourself and unborn child is to terminate the pregnancy. How would you feel when the child is born, and you have to watch her deteriorate and die after so much suffering. The likelihood of your child being born HIV negative is nil.” The woman refused to terminate, and today her child is nearly a teenager, HIV negative, and healthy.
Another woman, after missing a scheduled hospital visit due to transport issues, was told, “You decided to go on and enjoy sex and have a baby while you knew you are HIV positive, and therefore it is entirely your fault for infecting the child, and failing to meet appointments – we will attend to you last.”
The attitudes of service providers, and people living with HIV, are both light years apart from where the facts now reside. Extensive scientific research, partly conducted in Zimbabwe, now shows that use of a condom during a sexual encounter, especially if the person with HIV is taking antiretroviral medication and thus able to maintain an undetectable viral load, makes transmission of HIV to someone else highly unlikely.
The problem is not just with health service providers however. The law and attitudes of lawyers also lag behind science. For services to be particularly responsive to the needs of people living with HIV, legislation and legal policies also need to be revised in line with the scientific evidence that is rapidly emerging from ongoing research. Even though HIV transmission in the above circumstances is now known to be highly unlikely, the Zimbabwe legislation still treats all HIV as highly contagious. For example, the Criminal Law Codification and Reform Act 23/2004, states “(2) For the purposes of this section—(a) the presence in a person’s body of HIV antibodies or antigens, detected through an appropriate test, shall be prima facie proof that the person concerned is infected with HIV”. There has been no revision to this law to reflect the significant advances in scientific knowledge, so this statement is used to support the continued erroneous belief that all people with HIV having sex are likely to transmit HIV; and it upholds the views that they should be criminalised.
HIV-related stigma has remained high in Southern Africa in general, and across the whole of the sub-continent. While there have been many advances made in knowledge and management of HIV, such that neither in sexual intercourse nor in childbirth should there any longer be a threat of transmission, many still continue to acquire HIV through lack of ability to negotiate condom use, or lack of access to ARVs when needed, and they continue to bear the brunt of the epidemic.
The burdens faced by women in relation to HIV have often been cited. These burdens feel so big that any woman who has responsibility for caring for a child understandably feels she is protecting the minor by refusing to have her/him tested for HIV, or by refusing to disclose the child’s HIV positive status, even to the child concerned. A caring healthcare worker may also feel like this if a minor approaches them seeking to be tested for HIV.
The many discussions taking place amongst HIV programme implementers on “when to disclose to a child” are troubling. The argument many have put forward is that the child may be too young to understand, or too immature to be able to handle the 'burden' of knowledge of their HIV status, or a parent or guardian’s status. The fact is that having HIV is still not discussed because it still bears an element of taboo. Despite the many advances in research that have shown that HIV is not a contagious disease that can be spread by casual contact, it seems that much of society has remained stuck in the mode when not much was known about HIV, and there was no treatment. It is also considered safer not to know one’s status than to know it and run the risk of being accused of knowingly “putting someone else at risk”.
Surely therefore what decision-makers should be asking, instead of “when to disclose to a child?” is “how to overcome the stigmatising attitudes we as healthproviders and law-makers hold and convey?”
If HIV is talked about as part of normal conversations in the home and in the school, and not as a "contagious disease", then the issue of when to disclose falls away. When I tested HIV-positive, I immediately disclosed to my brothers and sisters and their children. It became part of normal conversations, and when it came to the time when my baby started asking questions about my condition, it was easy for me to disclose my status to her. While she was tested at 18 months, when she turned seven she insisted on getting tested - it was something easy to do, and gave her reassurance as to her status.
As counsellors, we are all taught that “change starts from within each and every one of us: without changing ourselves we can’t change others”. Yet this is not a concept that is familiar to other service providers or to law-makers.
We need to rethink how we change the landscape in relation to HIV, so that lawyers and health providers alike actually believe in and act on the science themselves, rather than continuing to behave as if HIV was a highly contagious condition whose carriers should be shunned and punished. Researchers working in the field of HIV would be wise to make a direct intervention to challenge and change the attitudes and practices of the health systems at national, regional, and international levels, on the results of emerging scientific research and the implications.
And what about our children? Unless we all take steps to change our own attitudes and those of our healthworkers and lawyers, our children will continue to acquire HIV at birth, and will continue to grow up uninformed, untested and untreated. They will also become criminalised as they begin to have their own sexual relations when older. And they will get sick and die. Unless we act now to perform a u-turn in attitudes and practices, this legacy of shame and blame will continue and will be the heritage that we, women and men alike, bequeath our children. And that will be a disaster for us all.
I am one of the many women with HIV who are not attending the conference this week, owing to lack of funds. However I very much hope that the issues I have raised here will be addressed.
This article is part of 50.50's long running series on AIDS Gender and Human Rights. We are publishing articles daily during the 2014 World AIDS Conference in Melbourne July 20-25